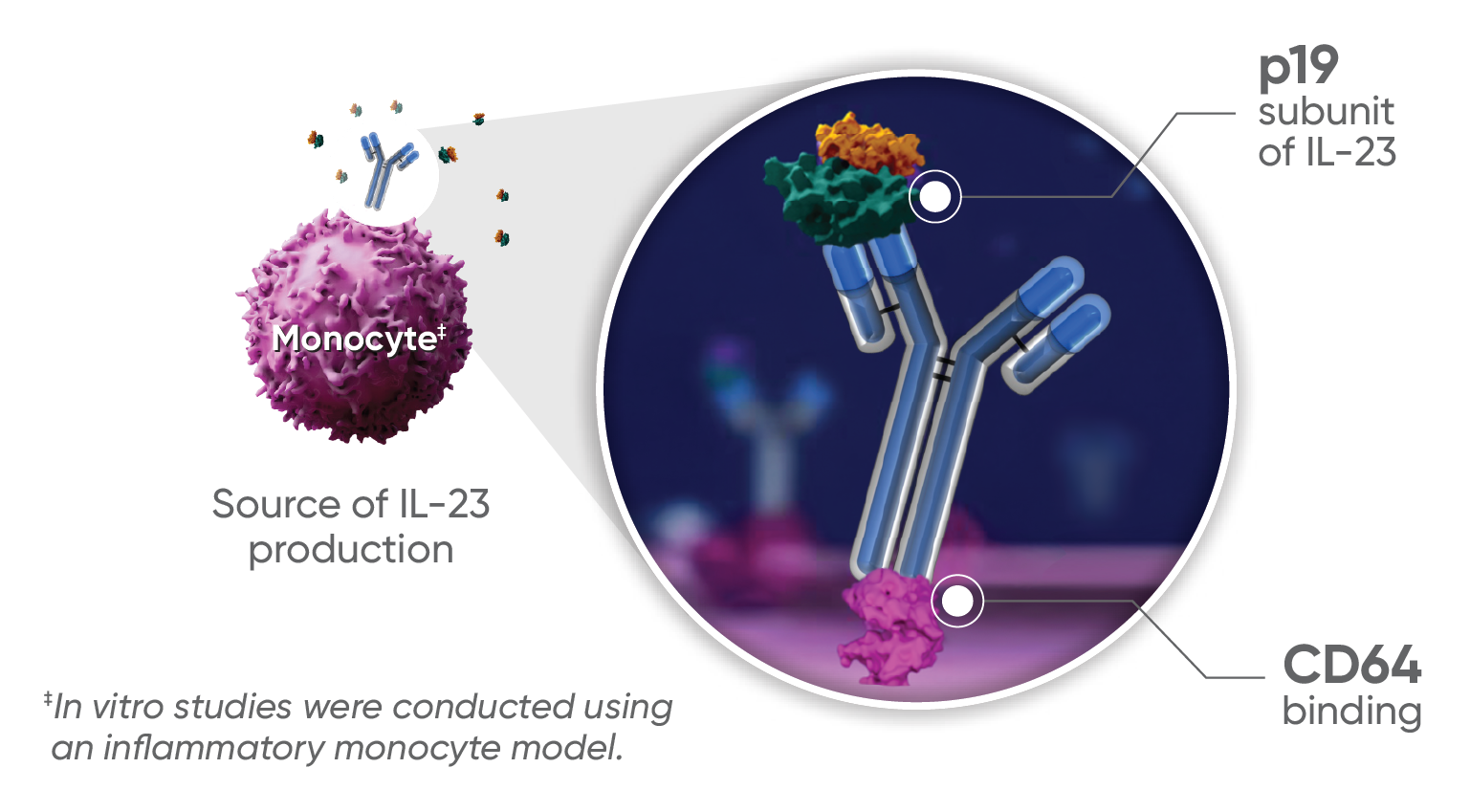
TREMFYA® is the only fully human anti–IL-23.
- IL-23 is a naturally occurring cytokine that is involved in normal inflammatory and immune responses1
- Interaction between IL-23 and its receptor drives the differentiation, proliferation, and survival of Th17 cells, which produce inflammatory cytokines4-6
- By blocking IL-23, TREMFYA® inhibits the release of important pro-inflammatory cytokines and chemokines4-6
- In evaluated subjects with plaque psoriasis, guselkumab reduced serum levels of IL-17A, IL-17F, and IL-22 relative to pretreatment levels based on exploratory analyses of the pharmacodynamic markers
- In evaluated subjects with psoriatic arthritis, serum levels of acute phase proteins, C-reactive protein, serum amyloid A and IL-6, and Th17 effector cytokines IL-17A, IL-17F, and IL-22 were elevated at baseline. Serum levels of these proteins measured at Week 4 and Week 24 were decreased compared to baseline following guselkumab treatment at Week 0, Week 4, and every 8 weeks thereafter
- The clinical significance of these findings is not known
The mean half-life of guselkumab in patients with plaque psoriasis: ~15 to 18 days.1
IL-23=Interleukin-23.
References: 1. TREMFYA® (guselkumab) [Prescribing Information]. Horsham, PA: Janssen Biotech, Inc. 2. Zhuang Y, Calderon C, Marciniak SJ Jr, et al. First-in-human study to assess guselkumab (anti-IL-23 mAb) pharmacokinetics/safety in healthy subjects and patients with moderate-to-severe psoriasis. Eur J Clin Pharmacol. 2016;72(11):1303-1310. 3. Data on file. Janssen Biotech, Inc. 4. Nestle FO, Kaplan DH, Barker J. Psoriasis. N Engl J Med. 2009;361(5):496-509. 5. Fitch E, Harper E, Skorcheva I, et al. Pathophysiology of psoriasis: recent advances on IL-23 and Th17 cytokines. Curr Rheumatol Rep. 2007;9(6):461-467. 6. Fujita H. The role of IL-22 and Th22 cells in human skin diseases. J Dermatol Sci. 2013;72(1):3-8.